by Dr. Sadiq Ali 6 June 2022
Monkeypox is a disease caused by the monkeypox virus. It is a viral zoonotic disease, meaning that it can spread from animals to humans. It can also spread between people. The disease is called monkeypox because it was first identified in colonies of monkeys kept for research in 1958. It was only later detected in humans in 1970.
Monkeypox is commonly found in central and west Africa where there are tropical rainforests and where animals that may carry the virus typically live. People with monkeypox are occasionally identified in other countries outside of central and west Africa, following travel from regions where monkeypox is endemic.
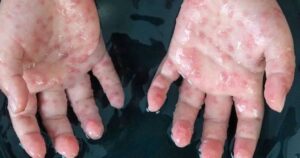
Symptoms of monkeypox typically include a fever, intense headache, muscle aches, back pain, lethargy, lymphadenopathy and a skin rash or lesions. The rash usually begins within one to three days of the start of a fever. Lesions can be flat or slightly raised, filled with clear or yellowish fluid, and can then crust, dry up and fall off. The number of lesions on one person can range from a few to several thousand. The rash tends to be concentrated on the face, palms of the hands and soles of the feet. They can also be found on the mouth, genitals and eyes. Symptoms typically last between 2 to 4 weeks and go away on their own without treatment.
Complications from severe cases of monkeypox include skin infections, pneumonia, confusion and eye infections which can lead to loss of vision. Around 3–6% of reported cases have led to death in endemic countries in recent times, often in children or persons who may have other health conditions. It is important to note that this may be an overestimate because surveillance in endemic countries is limited.
Monkeypox can spread to people when they come into physical contact with an infected animal. Animal hosts include rodents and primates. The risk of catching monkeypox from animals can be reduced by avoiding unprotected contact with wild animals, especially those that are sick or dead (including their meat and blood). In endemic countries where animals carry monkeypox, any foods containing animal meat or parts should be cooked thoroughly before eating. People with monkeypox are infectious while they have symptoms (normally for between two and four weeks). You can catch monkeypox through close physical contact with someone who has symptoms. The rash, bodily fluids (such as fluid, pus or blood from skin lesions) and scabs are particularly infectious. Clothing, bedding, towels or objects like eating utensils/dishes that have been contaminated with the virus from contact with an infected person can also infect others. Ulcers, lesions or sores in the mouth can also be infectious, meaning the virus can spread through saliva. People who closely interact with someone who is infectious, including health workers, household members and sexual partners are therefore at greater risk for infection.
There are several vaccines available for prevention of smallpox that also provides some protection against monkeypox. A newer vaccine that was developed for smallpox (MVA-BN, also known as Imvamune, Imvanex or Jynneos) was approved in 2019 for use in preventing monkeypox and is not yet widely available. WHO is working with the manufacturer to improve access.
Monkeypox symptoms often resolve on their own without the need for treatment. It is important to take care of the rash by letting it dry if possible or covering with a moist dressing to protect the area if needed. Avoid touching any sores in the mouth or eyes. Mouth rinses and eye drops can be used as long as cortisone-containing products are avoided. Vaccinia immune globulin (VIG) may be recommended for severe cases. An antiviral that was developed to treat smallpox (tecovirimat, commercialized as TPOXX) was also approved for the treatment of monkeypox in January 2022.
Since the current outbreaks began, some nations have been procuring smallpox vaccines, which are thought to be highly effective against monkeypox, because the viruses are related. Unlike some vaccines against COVID-19, which take up to two weeks after a second dose to offer full protection, smallpox vaccines are thought to protect against monkeypox infection if administered within four days of exposure because of the virus’s long incubation period, according to the US Centers for Disease Control and Prevention (CDC) .
- Further public health investigations are ongoing in non-endemic countries that have identified cases, including extensive case finding and contact tracing, laboratory investigation, clinical management and isolation provided with supportive care.
- Genomic sequencing, where available, have been undertaken to determine the monkeypox virus clade(s) in this outbreak
- Prevention – Someone who has direct contact with an infected person can get monkeypox. Steps for self-protection include avoiding skin to skin or face to face contact with anyone who has symptoms, keeping hands clean with water and soap or alcohol-based hand rub, and maintaining respiratory etiquette.
- Detection and care – If people develop a rash, accompanied by fever or a feeling of discomfort or illness, they should contact their health care provider and get tested for monkeypox. If someone is suspected or confirmed as having monkeypox, they should isolate until the scabs have fallen off .During this period, patients can get supportive treatment to ease monkeypox symptoms.
- Reporting – Any rash-like illness during travel or upon return should be immediately reported to a health professional, including information about all recent travel, sexual history and smallpox immunization history. Residents and travelers to monkeypox-endemic countries should avoid contact with sick mammals such as rodents, marsupials, non-human primates (dead or alive) that could harbour monkeypox virus and should refrain from eating or handling wild game (bush meat).
Clinical management and infection prevention and control
- Health workers caring for patients with suspected or confirmed monkeypox should implement standard, contact and droplet precautions. These precautions are applicable in any health facility including outpatient services and hospitals. Standard precautions include strict adherence to hand hygiene, appropriate handling of contaminated medical equipment, laundry, waste and cleaning and disinfection of environmental surfaces.
- Prompt isolation of suspected or confirmed cases in a single room with adequate ventilation, dedicated bathroom and staff is recommended. Cohort (confirmed with confirmed, suspected with suspected) can be implemented if single rooms are not available, ensuring minimum of 1-meter distance between patients. Recommended personal protective equipment (PPE) includes gloves, gown, medical mask and eye protection – goggles or face shield. The patient should also be instructed to wear a medical mask when they come into close contact (under 1m) with health workers or other patients, if they can tolerate it. Additionally, a bandage, sheet or gown can be used to cover lesions in order to minimize potential contact with lesions. PPE should be disposed of prior to leaving the isolation area where the patient is admitted.
- Aerosol generating procedures (AGPs) (i.e. aspiration or open suctioning of respiratory tract specimens, bronchoscopy, intubation, cardiopulmonary resuscitation), be required for any reason and cannot be delayed, then as a matter of standard practice, a respirator (FFP2 or certified N95) must be used by health care workers instead of a medical mask.
- Isolation and transmission-based precautions should be continued until resolution of symptoms (including the resolution of any rash and scabs that have fallen off and healed).
- Deployment of pharmaceutical countermeasures including specific antivirals (i.e. tecovirimat, which is approved for monkeypox, but not yet widely available) can be considered under investigational or compassionate use protocols, particularly for those who have severe symptoms or who may be at risk of poor outcomes (such as those with immune suppression).
The Government of Pakistan on Monday issued special instructions to all national and provincial health authorities to be on high alert concerning monkeypox and its close monitoring.